Tear in the Gestational Sac Is It Dangerour for Baby or Mom
Abstract
Our objective was to prospectively validate the use of gestational sac (GS), yolk sac (YS) diameter, crown-rump length (CRL), and embryonal eye charge per unit (HR) dimensions to place early on pregnancy loss. This was a prospective accomplice study of offset trimester pregnancies. GS and YS bore, CRL, and Hr measurements were serially obtained in singleton and twin pregnancies from vi through 10 weeks' gestation. Non-parametric tests and logistic regression models were used for comparisons of distributions and testing of associations. A total of 252 patients were included, of which 199 were singleton pregnancies, 51 were twins, and ii were triplets (304 full fetuses). Fifty-two patients had 61 losses. We built nomograms with the changes of the parameters evaluated in ongoing, likewise as in pregnancy loss. In the pregnancies which failed, all the parameters showed pregnant changes, with different temporal onsets: GS and YS were the beginning to become aberrant, deviating from normality as early on as 6 weeks' gestation (OR 0.01, 95% CI 0.0–0.09, and OR 3.36, 95% CI 1.53–seven.34, respectively), followed by changes in Hr, and CRL, which became evident at 7 and viii weeks (OR 0.96, 95% CI 0.92–1.0, and OR 0.59, 95% CI 0.48–0.73, respectively). Our observations showed that, later on 5 consummate weeks' gestation, a small GS and a big YS reliably predicted pregnancy loss. The YS reliably identified the occurrence of a miscarriage at to the lowest degree 7 days prior its occurrence. CRL and 60 minutes became abnormal at a later fourth dimension in pregnancy and closer to the outcome. These findings have of import implications for patient counseling and intendance planning, likewise as a potential bearing on cost effectiveness within early pregnancy intendance.
Introduction
Early on pregnancy loss - as well known every bit pregnancy loss, fetal demise, miscarriage, or spontaneous ballgame - is defined every bit a "nonviable, intrauterine pregnancy with either an empty gestational sac or a gestational sac containing an embryo or fetus without fetal centre activity prior to 12 weeks and 6 days of gestation"1. Information technology is the almost common complexity of early pregnancy, affecting about xxx% of pregnancies following assisted reproduction and ten% of spontaneously conceived pregnanciestwo,iii,four. The difference is explained by a later diagnosis of spontaneous pregnancy versus assisted reproduction pregnancy, and an early loss is easily overlooked. In fact, vaginal haemorrhage - a common sign of early on pregnancy loss - tin can be confused with delayed flow and the loss remains unrecognized. The most mutual crusade of a first trimester pregnancy loss is embryonal genetic abnormalities, which occurs in more l% of the cases, with aneuploidy being the nigh frequent abnormalityfive,vi.
Multiple serologic and ultrasound markers have been investigated to identify pregnancies destined to be lost7,8. However, serologic markers are unspecific and can help only later on a pregnancy loss has already been diagnosed. Transvaginal ultrasound (TVUS) provides high-resolution images, low inter-observer variability with loftier reliability, and is typically used to make diagnosis of intrauterine pregnancy and to follow up with its evolution9. Gestational sac (GS), yolk sac (YS), crown-rump length (CRL), and heart rate (Hour) are the parameters measured to evaluate early pregnancy. Deviations in the ultrasound parameters have been alternatively investigated to predict beginning trimester pregnancy loss. The amniotic sac, which becomes visible at the beginning of the 7th week of gestation, is normally non contemplated in the prediction models, yet it assists in dating a pregnancy correctly.
Logistic models have been used to assess predictability of pregnancy loss using ultrasound parameters equally dependable variables. One model including 566 gravidas, 7.9% of whom had an early pregnancy, identified Hr and CRL every bit the most significant parameters to predict a pregnancy loss, together with maternal age and vaginal haemorrhage8. Another 1 evaluated pregnancies accomplished by in vitro fertilization and constitute that multiple variables including maternal age, duration of infertility, GS diameter, CRL, HR, and YS, predicted an early pregnancy loss better than each private parameters10. Even so, the model did not include an exact gestational age and included variables, such as maternal historic period, which lone is a well-established gamble factor for get-go trimester pregnancy loss11. Another model reported that a CRL, GS, and Hr, beneath the fiveth percentile, and a YS bore in a higher place the 95th percentile would predict early on pregnancy loss (odds ratio 1.04). Notwithstanding, a normal YS would not decrease the risk of pregnancy loss when the other parameters were abnormal12. A systematic review evaluated sensitivities and specificities of the ultrasound parameters and establish that 60 minutes ≤ 110 beats per minute (BPM) was the well-nigh reliable model to predict a subsequent pregnancy loss, with a sensitivity of 68.4%, a specificity of 97.eight%, a positive likelihood ratio of 31.7 (95% confidence interval 12.8–78.8), and a negative likelihood ratio of 0.32 (95% confidence interval 0.16–0.65). In pregnancies with vaginal bleeding, in addition to an HR ≤ 110 BPM, prediction of an early on loss was higher13. All the discussed early on pregnancy ultrasound markers have been alternatively found to predict first trimester loss, however they have never been evaluated longitudinally, and simply i ultrasound per patient was included in the analyses10,13,xiv,fifteen.
The yolk sac has been individually studied equally a marker of pregnancy loss. Being identified at approximately 5 weeks of gestation and gradually increasing in size in a linear manner until 10 weeks of gestation, the YS is the get-go identifiable structure via transvaginal ultrasonography within the GS. In particular, a YS larger than six.0 mm at any gestational age was associated with early loss, while an abnormal shape would not carry an ominous prognosis15,sixteen. Our group established a nomogram of YS growth from its first appearance until 10 weeks of gestation and found that deviations from the typical growth pattern were associated with a pregnancy loss17.
Previous studies were cross sectional and provided estimates for pregnancy loss that were based on a combination of ultrasound, every bit well as serologic and demographic markers. The aim of this study was to estimate a risk of first trimester pregnancy loss based solely on ultrasound findings. Thus, we longitudinally evaluated the GS, YS, CRL, and Hr changes in singleton and multiple pregnancies with definite conception dates in order to build nomograms of their changes up to 10 weeks of gestation. In improver, we wanted to identify which parameters were the commencement and almost reliable to predict a pregnancy loss in singleton and multiple pregnancies. Our hypothesis was that unlike markers would sequentially become abnormal at different embryonal stages, when a pregnancy is destined to be lost.
Materials and Methods
This was a prospective cohort report. The conduct of this study was approved by the Academy of Tennessee Health Science Center Human Investigation Committee and the study is currently registered at ClinicalTrials.gov (NCT02429336). All methods were performed in accordance with the relevant guidelines and regulations. All patients gave informed, written consent to participate in the study. The patients in our study were all evaluated and treated for infertility and had known formulation dates. The mode of conception included spontaneous, subsequently superovulation with clomiphene citrate or letrozole with, or without, intrauterine insemination (IUI), and in vitro fertilization (IVF) after superovulation with gonadotropins. The GS and YS bore, CRL, and HR measurements were obtained with ii-D transvaginal ultrasound in singleton, and multiple pregnancies followed from vi through 11 weeks' gestation. For the scans we used two ultrasound machines: Philips XD11 with a 7.5 MHz transvaginal probe and a Samsung UGEO WS80A 3-D with a 7.5 MHz transvaginal probe. All measurements were obtained on a magnified, frozen section (sagittal and/or transverse) of the parameter to exist evaluated. Measurements of the GS were obtained in three dimensions (length, height, width), the YS diameter was measured from one inner rim to the contrary inner rim. If not spherical, the iii dimensions were measured and averaged. The CRL was measured once and the FHR was measured once with M mode. Both parameters' measurements were repeated in different sections if the offset measurement did not meet the expected value for gestational age. The ultrasound auto provides the expected gestational age for each variable measured based on standardized algorithms, except for YS. For YS, we used the previously established nomogram of YS growth from 5 until x weeks of gestation17. Figure 1 shows the right cursor position for the measurement of the parameters under investigation. The GS largest diameter was measured in the three orthogonal planes and averaged (Fig. 1A). The YS largest diameter was measured placing the calipers at the inner rim of the organ. CRL was measured placing the calipers in the most cephalad and nigh caudal extremities of the embryo's longitudinal image. HR was automatically calculated by the car, averaging the distance between i, or two, systolic spikes.
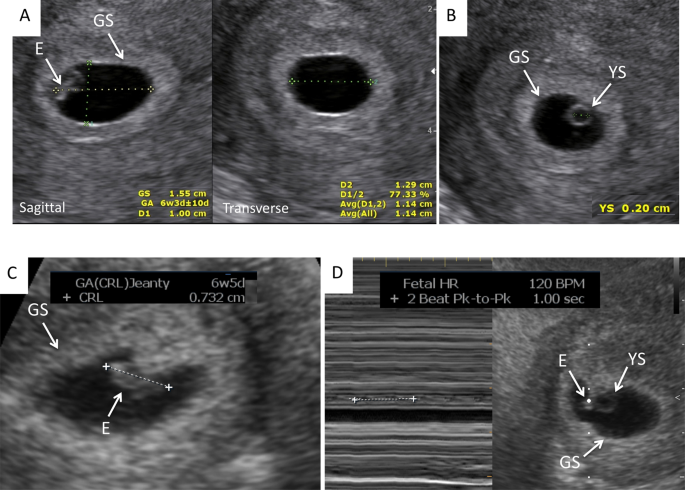
Correct cursor position for the measurement of the parameters under investigation: (A) Gestational sac (GS); (B). Yolk sac (YS); (C). Crown-rump length (CRL); (D). Middle Charge per unit (HR). E = Embryo.
All the clinic patients with a positive pregnancy examination were invited to come to the dispensary for an initial transvaginal ultrasound at five–six weeks of gestation, depending of the patient's history. All patients presenting between January 2014 and December 2017 were included in the study. Most patients had weekly ultrasounds from five to xi weeks of gestation, for an average of 4 scans per patient. To maintain consistency, a single examiner performed all of the sonographic exams of this written report. If at the initial scan the embryo had no cardiac action, all parameters were measured to confirm the gestational historic period and a 2nd scan was performed 1 week later on to ostend the result. If no gestational sac was nowadays, and an ectopic pregnancy was excluded, or the mean gestational sac diameter measured more than 20 mm without a visible YS or embryonal pole, these were classified as a nonviable pregnancy and were excluded from the analyses. In this cohort, there were no pregnancies that ended in elective termination.
Recurrent pregnancy loss was divers as 2 or more outset trimester pregnancy lossesxviii. All pregnant women were discharged from the Reproductive Medicine clinic between x and xi weeks of gestation. Pregnancy result was determined through the evaluation of hospital medical records.
Statistical analysis
Variables, fifty-fifty if continuous, were expressed as Median and quartiles (Q1, Q3) because the Median is not skewed so much by a pocket-size proportion of extremely large or small values and it is more than representative of a typical value. All analyses were performed using SAS/STAT V14.1 (Cary, Due north Carolina, USA). Mann-Whitney U test and Pearson correlations were used for comparisons between the ongoing pregnancy and pregnancy loss groups (Table 1). The GS and YS diameters, CRL and FHR were plotted relatively to gestational age. Descriptive statistics including medians and quartiles for GS, YS, CRL and Hr for each gestational calendar week were calculated by pregnancy loss condition. If a patient had a loss before and a continuing pregnancy after, she was allocated to the group which identified the outcome at the time of her pregnancy. If the patient had twins, or triplets, with one or ii losses within the aforementioned pregnancy (=vanishing twin), to balance the results she was allocated to both groups. Nosotros applied Wilcoxon ii-sample tests past gestational week for univariate comparison of distributions/medians for GS, YS, CRL, and HR, between the pregnancies that were lost and those that were not. For YS, we as well performed a median split analysis using Wilcoxon 2-sample tests by gestational calendar week both above and below the YS median, to compare the YS medians by pregnancy loss status. We calculated the gestational historic period in weeks, rather than in days, because it is the standard method to measure the gestational age in clinical practice. Nosotros extended the univariate analysis into multivariate logistic regression models in club to retain multiple significant predictors of pregnancy loss by gestational calendar week. Non-significant variables were omitted from the model unless contributing to the overall fit of the model. We estimated optimal sensitivity and specificity of each model along with area under the receiver operating characteristic bend (AUC). All associations were considered significant at alpha level 0.05.
Results
Of the 252 pregnancies included in this study, 199 (78.nine%) were singleton pregnancies, 51 (20.2%) were twins (iii of which were monochorionic and 48 dichorionic), and 2 (0.008%) were triplets (monochorionic twins plus a singleton; both pregnancies spontaneously reduced to singleton at 7 weeks of gestation), for a total of 304 embryos longitudinally studied (one of the twin pregnancies had an empty GS, which was excluded from the calculations). Thirty-six of 252 pregnancies (fourteen.iii%) had a first ultrasound between four–v weeks of gestation because of history of ectopic pregnancy, recurrent pregnancy loss, pelvic pain, or vaginal haemorrhage. For 21 patients, no delivery information was available, however they were lost to follow-upwards later their third-trimester ultrasound and were included in the analyses in the grouping of patients who had a continuing pregnancy.
Threescore-one of 304 (20%) embryos, in 52 pregnancies, were lost: 20/61 (32.8%) in twin, or triplet, pregnancies and 41/61 (67.ii%) in singleton pregnancies. The remaining 243 embryos progressed beyond the first trimester. Thirty-three of 61 embryos (54.1%) were already lost at the fourth dimension of the initial ultrasound, of which 19 (31.one%) at four–v weeks and 14 (22.9%) at half dozen weeks of gestation. Of the pregnancies that were lost, just 5 had vaginal bleeding every bit the initial sign of pregnancy failure, all in singleton pregnancies. Neither of the twin pregnancies with a vanishing or demised twin underwent genetic analysis. Of the 61 pregnancy losses, xviii singleton and 1 twin pregnancies underwent microarray analysis for genetic aberration: results were inconclusive in two instances, and unknown in 1. Twelve of 17 (70.six%) showed chromosomal abnormalities: 4 were trisomy 21, 2 were trisomy 16, 2 were trisomy 22, two were triploid, and 2 were complex genetic abnormalities. All embryos had a YS diameter larger than the median in continuing pregnancies pregnancies. V of 17 (29.four%) were normal karyotypes and all embryos had smaller or similar YS diameter compared to the median in continuing pregnancies.
Table 1 reports the demographics and the clinical characteristics of patients that had a first trimester pregnancy loss (N = 52, 61 lost embryos) and those who connected the pregnancy across the kickoff trimester (N = 209, 243 fetuses). Variable measurements in the standing pregnancy grouping conformed to the expected value by gestational age calculated by the ultrasound machine and were considered the normal cut-offs at each gestational historic period. Patients with twin/triplet pregnancies who lost one, or two, embryos, only continued the pregnancy with the remaining fetus/es (thirteen/51 twins and ii/2 triplets) were allocated to both groups. In this way, maternal characteristics would have the same statistical weight in the two groups. There was no difference in age, BMI, gravidity, parity, mode of formulation, and clinical history (all not significant to <0.05). Spontaneous formulation was the most mutual manner of conception in the pregnancy loss group, while IVF was the most common in the continuing pregnancy group; polycystic ovary syndrome was the most common preexisting clinical status in both groups, followed by uterine subseptations. Seventy-one patients had had one, or two, pregnancy losses prior to the alphabetize pregnancy. Twenty-half-dozen patients had a diagnosis of recurrent pregnancy loss (6 in the pregnancy loss, and 20 in the continuing pregnancy group). 2 twin pregnancies were delivered at 26 weeks of gestation: one for preterm delivery and the other for astringent preeclampsia in a 44 year-old woman who had conceived through egg donation. 1 singleton pregnancy was included in the standing pregnancy group even though it was complicated by fetal demise at 24 weeks from a tight nuchal string. The fetus had a normal male karyotype, 46, XY. Fifty-viii additional fetuses were delivered between 32 and 36 six/vii weeks of gestation, mostly from preterm commitment of twin pregnancy (45 fetuses in twin pregnancies, and 13 fetuses in singleton pregnancies), and the remaining 180 fetuses were delivered at term (≥37 weeks of gestation). None of the neonates had genetic abnormalities. All the investigated parameters became significantly different in pregnancies destined to exist lost, but with a different chronology. Aside from the GS dimensions in monochorionic twins, in that location was no difference in dimension of whatever other parameters in singleton versus multiple pregnancies.
Effigy ii shows the median GS, YS, CRL, and 60 minutes measurements at the gestational ages under investigation in the two groups, pregnancy loss and continuing pregnancy. Variable measurements in the standing pregnancy group conformed to the expected gestational age by the ultrasound car and were considered the normal cutting-offs at each gestational historic period. The GS diameter grew 6.65 mm per week (Rtwo = 0.9979) in pregnancies that continued across the get-go trimester and information technology was smaller in pregnancies destined to be lost, nonetheless the difference was not significant until 8 weeks of pregnancy, when the median bore of the gestational sac was 15 mm (IQR 12, 21 mm) in pregnancy losses and 31 mm (28, 35 mm) in continuing pregnancies (p < 0.001, Fig. 2A, Table 2). The YS grew 0.38 mm per week (R2 = 0.9983) in pregnancies that continued beyond the first trimester. In pregnancies destined to be lost, the YS was either smaller, or larger, than in continuing pregnancies starting at 5 weeks of gestation, and maintained the trend until the pregnancy loss was diagnosed (Fig. 2B, Table ii). The CRL grew 7.54 mm (R2 = 0.9903) per week and was significantly larger in the standing pregnancy than in the pregnancy loss grouping from 6 through 10 weeks (Fig. 2C, Table 2). HR increased from 5 weeks of gestation and became significantly different in the two groups betwixt 7 and 8 weeks of gestation, when it increased past xiii BPM in the continuing pregnancy, versus increasing 3 BPM in the pregnancy loss grouping. 60 minutes still fit a linear relationship with gestational age, increasing by 13.76 BPM per week, fifty-fifty though with a lower Rii of 0.8637.
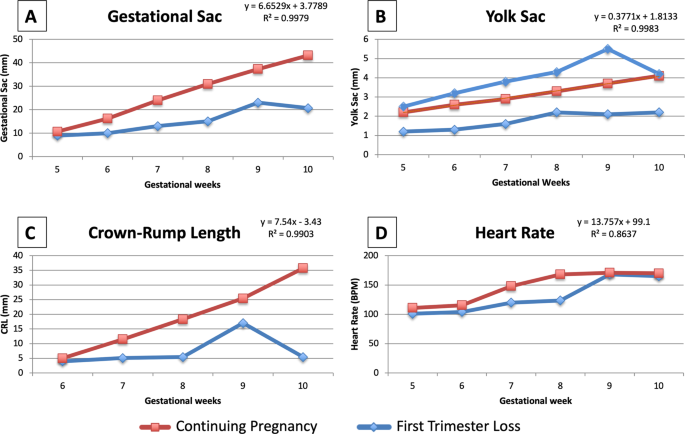
Median measurements of the parameters nether investigation in the two groups, pregnancy loss and continuing pregnancy, plotted against the gestational age: (A). Gestational sac (GS); (B). Yolk sac (YS); (C). Crown-rump length (CRL); (D). Eye Rate (HR).
Univariate comparisons are reported in Table ii. In early gestational weeks (weeks 7 and eight), a larger median YS was associated with an increased take a chance of pregnancy loss, whereas in calendar week 10, a smaller median YS was associated with an increased take chances of pregnancy loss. Starting at 6 weeks of gestation up to 10 complete weeks, smaller GS and CRL were associated with a subsequent pregnancy loss (p < 0.01 for all). A slower HR was predictive of a subsequent pregnancy loss at vii through 8 weeks of pregnancy (p < 0.05 for both), however, this did not hold truthful for a slower HR occurred prior to vii weeks or afterwards viii weeks.
This analysis further confirmed our findings when we subdivided the pregnancy loss grouping into those below and above the expected YS median per gestational age. In fact, a smaller YS diameter was associated with pregnancy loss at week six (tendency), and eight–10 of gestation (p < 0.05 for all), and a larger YS diameter was associated with pregnancy loss from week 6–9 of gestation (p < 0.05 for all; Tabular array 3). Figure 2B reports the YS bore of pregnancy losses at different gestational ages compared to continuing pregnancies. Figure 3 shows ultrasound and hysteroscopic images of an enlarged YS in a 69, XXY pregnancy. Using the significant univariate models and subsequently excluding 19 pregnancy losses diagnosed at the time of the initial ultrasound, 43% of the losses (18/42) could be predicted at to the lowest degree ane week earlier they occurred. In item, a smaller GS, a shorter CRL, and a larger YS, could predict 43% of the pregnancy losses one calendar week in advance in ix cases, 2 weeks in advance in 7 cases, 3 weeks in accelerate in 1 instance, and v weeks in advance in ane case. A slow embryonal Hr was not amply anticipatory of a loss.

(A) Ultrasound and hysteroscopic images of the yolk sac in a partial mole pregnancy (Karyotype: 69, XXY at microarray analysis). (A) Ultrasound moving-picture show showing an enlarged yolk sac at 6 weeks and one day of gestation; (B). Ultrasound picture showing an enlarged yolk sac at eight weeks and 2 days of gestation; (C). Hysteroscopic view of the yolk sac at the fourth dimension of pregnancy evacuation at 8 weeks and 2 days of gestation, after embryonal demise. (D) A portion of the yolk sac tin can be noted just outside of the amniotic sac, with the embryo within it, in the background. GS = gestational sac; YS = yolk sac.
Results of the logistic regression models for the multivariate assay are displayed in Table 4. These regressions were performed past gestational week, with pregnancy loss as the effect variable. Sensitivity and specificity were estimated from the models, AUC is presented every bit a mensurate of model fit. These adapted models largely confirm the univariate findings. A larger YS was associated with a 3–6 times increased chance of pregnancy loss from 5 through 8 weeks. At ten weeks of gestation, instead, a larger YS was associated with a decreased chance of pregnancy loss. This is reflected in the fact that simply ane pregnancy loss after 10 weeks of gestation had an enlarged YS. In fact, all the losses at that gestational historic period showed a YS smaller than the median for pregnancies continuing across the starting time trimester. A larger GS was associated with a decreased run a risk of losing the pregnancy, suggesting that a smaller GS, instead, is indicative of pregnancy loss. The direction of this association was consistent over the time frame under investigation, reaching significance at, half-dozen, 7, and 9 weeks. Similarly, a larger CRL measurement was associated with a decreased adventure of pregnancy loss, again indicating that a smaller CRL at 8 and 9 weeks of gestation predicts a pregnancy loss. The models performed with reasonable predictive accuracy and goodness of fit. Sensitivity ranged from 60–86% and specificity from 78–91%.
Discussion
In pregnancies destined to be lost, dissimilar ultrasound markers became abnormal at to the lowest degree 1 calendar week before the loss. We established that the GS, CRL, and YS are the start parameters to get abnormal, as early as 5 weeks of gestation, and that HR becomes aberrant at a later time and simply for a brief period prior to the loss. In addition, multiple markers predict the outcome with increased sensitivity and specificity compared to each individual marker.
The pregnancy loss rate of 20% in our study was comparable to the one reported for IVF2, but college than the i reported for spontaneous pregnancies (well-nigh 10%)3,4. However, in our cohort almost losses occurred inside fourteen days of the missed menses, and in unlike circumstances where the formulation date is not known, a pregnancy, and hence a pregnancy loss, would about often go unrecognized. The fact that spontaneous conception was the most common mode in the pregnancy loss grouping, while IVF was the most mutual in the continuing pregnancy group could be due to the unlike support of the luteal phase and early on pregnancy stages, as IVF pregnancies are supported with gonadotropins prior to, and progesterone after, the 24-hour interval after oocyte retrieval (corresponding to the day of ovulation in spontaneous pregnancies), which change the endometrial characteristics compared with spontaneously conceived pregnancies. Polycystic ovary syndrome was the virtually common preexisting clinical condition in both groups; it was treated in all patients with daily metformin, 500 mg to 2000 mg. These results might help understanding the etiology of pregnancy loss in women with this condition, which in our study, seemed to be unrelated to the hyperinsulinemic condition, often reported as the about probable cause of pregnancy loss19. However, studies powered to explore our incidental finding would be needed.
The YS appeared to be the strongest mark for the prediction of a pregnancy loss. Other studies have established YS every bit a reliable predictor of pregnancy outcome, still these studies are limited by their cross-sectional evaluation with only ane ultrasound per patientten,12,13,fourteen,15,16. In our study we performed multiple ultrasounds to accurately stand for all gestational ages in each patient. Nosotros previously described a nomogram of YS development during the first ten weeks of pregnancy with serial ultrasounds in pregnancies that continued beyond the first trimester17. Nosotros confirmed a YS linear growth of approximately 0.four mm per week in this larger patient sample. Our findings corroborate a large cross sectional study with over four,000 patients20. Subsequently v consummate weeks of gestation, the YS reliably detects pregnancies destined to exist lost, as well confirmed by multivariate assay. In pregnancies destined to fail, the YS was either smaller or larger than in pregnancies continuing beyond the offset trimester. While all pregnancies with a large YS were lost within x weeks, some pregnancies with smaller YS were lost beyond 10 weeks of pregnancy. The etiology of a big YS is essentially unknown, however 18–66% of big YS diameters greater than v–6 mm have been associated with aberrant karyotypes21,22. Our express genetic results seem to corroborate these previous findings.
CRL is difficult to mensurate at 6 weeks of gestation, being subject field to the sonologist's feel and the ultrasound automobile'southward capabilities. Several nomograms for CRL accept been developed in different countries past cross sectional studies. An international nomogram of CRL growth was recently developed for pregnancy dating, however measurement started at 9 weeks of gestation23. Between 6 and 10 weeks of gestation, some other cantankerous sectional report found a quadratic relationship between CRL and gestational age20. Our results, dating from 5 weeks of gestation, defined a linear fit of CRL growth, up to ten weeks. CRL was a weak predictor of pregnancy loss between 6 and 8 complete weeks of gestation, however it became a stronger predictor when combined with YS or GS abnormalities. In addition, the growth lag ordinarily preceded the issue by less than one week, thus providing niggling fourth dimension for counseling.
Many Hr nomograms have been developed, and one with the largest data was by Papaioannoutwenty. In this cross sectional study a cubic association between HR and gestational age was found. However those pregnancies were followed through xiii weeks of gestation, when a natural slowing in HR is observed. We described a linear relationship through 10 weeks of gestation with an excellent Rtwo value. Given the rather important variation in BPM per second, a slower HR is non a reliable tool to predict the occurrence of a pregnancy loss unless it is below 100 BPM at a gestational age greater than 6 weeks of gestation24. In our written report, a HR slower than in continuing pregnancies was predictive of a subsequent pregnancy loss only between 7 and viii weeks of gestation, but not prior, or afterwards, this time. Even if highly specific of pregnancy loss when absent, HR abnormalities presented very shut to the upshot, thus providing little time for counseling.
A major forcefulness of our study is the advantage of a single investigator performing all the ultrasounds, thus maintaining consistency in the measurements, with pocket-size inter-observer variability. Additionally, all subjects included in the report had precisely known gestational ages further strengthening the accuracy of our results. Limitations of the report include the relatively small sample size, along with a patient population treated for infertility, which may make our results not generalizable to spontaneous conceptions. Additionally, some pregnancies were already lost at the time of the first ultrasound at v or half dozen weeks of gestation, and we were non able summate the interval between the measured abnormal parameter and the loss. In fact, our model was suitable mostly for pregnancies that had an ultrasound at 6 weeks and were lost at 8–9 weeks of gestation, or after. Nosotros analyzed the data 'per week' of gestation to reverberate the standard gestational age quantification, however, we may have lost sharpness of the results every bit compared to analyzing the information 'per day' of gestation.
In conclusion, we were able to found a statistical model using merely early pregnancy ultrasound markers to predict a first trimester loss. GS and YS were the earliest parameters that could reliably be used as prognostic factors for pregnancy loss, as they became abnormal as early as six weeks of gestation with high sensitivity and specificity. Of all the evaluated parameters, the YS was the strongest single predictor. These findings are clinically useful for patient counseling and determining the need for closer monitoring. In fact, if these parameters are normal at 6 weeks, the pregnancy will probable continue beyond the get-go trimester. Although needing prospective validation, our results support changing the current standard of intendance of performing the commencement obstetric ultrasound at ix weeks of gestation to 6 weeks of gestation. If the YS and the GS are normal, a provider can offering reassurance concerning the decreased likelihood of a pregnancy loss.
Alter history
-
28 Oct 2021
A Correction to this paper has been published: https://doi.org/x.1038/s41598-021-01235-0
References
-
American Higher of Obstetricians and Gynecologists. Early pregnancy loss. Practice Bulletin No. 150. Obstet & Gynecol 2015; 125, 1258–1267. Retrieved February 15, 2018, from, http://www.acog.org/Resources-And-Publications/Practice-Bulletins/Committee-on-Practice-Bulletins-Gynecology/Early-Pregnancy-Loss.
-
Orvieto, R. et al. Outcome of pregnancies derived from assisted reproductive technologies: IVF versus ICSI. J Assist Reprod Genet 17, 385–387 (2000).
-
Wang, X. et al. Conception, early pregnancy loss, and time to clinical pregnancy: a population-based prospective written report. Fertil Steril 79, 577–84 (2003).
-
Zinaman, K. J., Clegg, East. D., Brown, C. C., O'Connor, J. & Selevan, Due south. Thousand. Estimates of homo fertility and pregnancy loss. Fertil Steril 65, 503–9 (1996).
-
Lathi, R. B. & Milki, A. A. Tissue sampling technique affects accurateness of karyotype from missed abortions. J Assist Reprod Genet nineteen, 536–538 (2002).
-
Zhang, H. One thousand. et al. Analysis of fetal chromosomal karyotype and etiology in 252 cases of early spontaneous abortion. Zhonghua Yi Xue Yi Chuan Xue Za Zhi 28, 575–578 (2011).
-
Lek, S. Grand. et al. Validation of serum progesterone <35 nmol/Fifty as a predictor of miscarriage among women with threatened miscarriage. BMC Pregnancy Childbirth 17, 78–84 (2017).
-
Tarasconi, B. et al. Serum antimüllerian hormone levels are independently related to miscarriage rates after in vitro fertilization-embryo transfer. Fertil Steril 108, 518–524 (2017).
-
Pexsters, A. et al. Clinical implications of intra- and interobserver reproducibility of transvaginal sonographic measurement of gestational sac and crown-rump length at 6–9 weeks' gestation. Ultrasound Obstet Gynecol 38, 510–5 (2011).
-
Yi, Y. et al. A logistic model to predict early pregnancy loss following in vitro fertilization based on 2601 infertility patients. Reprod Biol Endocrinol 14, 15 (2016).
-
Khalil, A., Syngelaki, A., Maiz, North., Zinevich, Y. & Nicolaides, K. H. Maternal age and adverse pregnancy outcome: a accomplice study. Ultrasound Obstet Gynecol 42, 634–43 (2013).
-
Datta, M. R. & Raut, A. Efficacy of start-trimester ultrasound parameters for prediction of early spontaneous abortion. Int J Gynaecol Obstet 138, 325–330 (2017).
-
Pillai, R. N., Konje, J. C., Richardson, M., Tincello, D. Chiliad. & Potdar, N. Prediction of miscarriage in women with viable intrauterine pregnancy—A systematic review and diagnostic accurateness meta-analysis. Eur J Obstet Gynecol Reprod Biol 220, 122–131 (2018).
-
Stamatopoulos, N. et al. Prediction of subsequent pregnancy loss gamble in women who nowadays with a viable pregnancy at the first early pregnancy browse. Aust N Z J Obstet Gynaecol 55, 464–72 (2015).
-
Tan, S. et al. Abnormal sonographic appearances of the yolk sac: which can be associated with adverse perinatal effect? Med Ultrason sixteen, xv–twenty (2014).
-
Ashoush, S., Abuelghar, W., Tamara, T. & Aljobboury D. Relation betwixt types of yolk sac abnormalities and early on embryonic morphology in showtime-trimester missed pregnancy loss. J Obstet Gynaecol Res., 42(1), 21–8, https://doi.org/10.1111/jog.12837 (2016 Jan).
-
Detti, L. et al. Pilot study establishing a nomogram of yolk sac growth during the start trimester of pregnancy. In Printing, Journal of Obstetrics and Gynecology Research (2019).
-
Definitions of infertility and recurrent pregnancy loss: a committee opinion. Fertil Steril, 99, 63 (2013).
-
Goodman, Due north. F. et al. American Association of Clinical Endocrinologists (AACE); American Higher of Endocrinology (ACE); Androgen Backlog and PCOS Society. American association of clinical endocrinologists, American college of endocrinology, and Androgen Excess and PCOS Gild illness state clinical review: Guide to the best practices in the evaluation and treatment of polycystic ovary syndrome - Part 2. Endocr Pract 21, 1415–26 (2015).
-
Papaioannou, G. I., Syngelaki, A., Poon, 50. C., Ross, J. A. & Nicolaides, Thousand. H. Normal ranges of embryonic length, embryonic eye charge per unit, gestational sac diameter and yolk sac diameter at 6-10 weeks. Fetal Diagn Ther 28, 207–xix (2010).
-
Goldstein, Due south. R., Kerenyi, T., Scher, J. & Papp, C. Correlation betwixt karyotype and ultrasound findings in patients with failed early on pregnancy. Ultrasound Obstet Gynecol viii, xiv–317 (1996).
-
Yoneda, S. et al. A Yolk Sac Larger Than 5 mm Suggests an Abnormal Fetal Karyotype, Whereas an Absent Embryo Indicates a Normal Fetal Karyotype. J Ultrasound Med 37, 1233–41 (2018).
-
Papageorghiou, A. T. et al. International Fetal and Newborn Growth Consortium for the 21st Century (INTERGROWTH-21st). International standards for early fetal size and pregnancy dating based on ultrasound measurement of crown-rump length in the starting time trimester of pregnancy. Ultrasound Obstet Gynecol 44, 641–8 (2014).
-
Doubilet, P. M., Benson, C. B. & Chow, J. South. Long-term prognosis of pregnancies complicated by slow embryonic heart rates in the early first trimester. J Ultrasound Med eighteen, 537–41 (1999).
Acknowledgements
This report was supported by an institutional grant from the University of Tennessee Health Scientific discipline Center, Memphis, TN (E07-3225-001).
Author information
Affiliations
Contributions
L.D. Research idea, Figures, Tables, Manuscript writing. L.F., M.Due east.C. and I.P.-A. Enquiry conduct, Manuscript writing.. P.J.G. Statistical analysis, Tables, Manuscript writing. Z.B. Statistical analysis. R.A.R. Research conduct, Manuscript writing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Boosted information
Publisher's note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The original version of this Article contained an error in the spelling of the author Patricia J. Goedecke which was incorrectly given as Patricia J. Goeske.
Rights and permissions
Open up Access This commodity is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in whatever medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were fabricated. The images or other third party material in this commodity are included in the article's Creative Commons license, unless indicated otherwise in a credit line to the cloth. If cloth is not included in the commodity's Creative Commons license and your intended apply is not permitted by statutory regulation or exceeds the permitted use, you lot will demand to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/past/four.0/.
Reprints and Permissions
About this article
Cite this article
Detti, L., Francillon, L., Christiansen, 1000.Due east. et al. Early pregnancy ultrasound measurements and prediction of starting time trimester pregnancy loss: A logistic model. Sci Rep x, 1545 (2020). https://doi.org/ten.1038/s41598-020-58114-3
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1038/s41598-020-58114-3
Further reading
Comments
By submitting a annotate you concur to abide by our Terms and Community Guidelines. If you discover something calumniating or that does not comply with our terms or guidelines please flag information technology as inappropriate.
Source: https://www.nature.com/articles/s41598-020-58114-3?error=cookies_not_supported&code=51684c7e-d7cd-4c70-be52-b8514a3ced16
0 Response to "Tear in the Gestational Sac Is It Dangerour for Baby or Mom"
Postar um comentário